Feline Stomatitis: What It Is, How It’s Treated, and What to Expect
Feline stomatitis is one of the most painful conditions a cat can experience, yet it often goes unnoticed at first. Many cats become quieter about their discomfort. They may hesitate at the food bowl, drop kibble, drool more than usual, or pull away from interaction. Subtle changes like these are easy to miss, especially in cats who are naturally reserved. If something about your cat’s eating habits or behavior feels off, their mouth may be the reason. Understanding the signs early can make a meaningful difference in their comfort and quality of life.
Just Cats Clinic in Reston, VA is a Certified Cat-Friendly, AAHA-accredited practice with expert dentistry services and the clinical expertise to guide you through every step of stomatitis care. If you have concerns about your cat’s mouth, contact our hospital to get started.
Is Your Cat Turning Away from Their Food Bowl?
It can start quietly. Your cat walks up to their bowl, takes a sniff, and walks away. Perhaps they are drooling more. Maybe their coat has gotten rougher, or they’ve started hiding more than usual.
These aren’t random signs of getting older. They’re often early clues that something serious is going on inside your cat’s mouth, and they deserve a closer look.
What Exactly Is Feline Stomatitis?
Feline chronic gingivostomatitis (FCGS) is a condition where the body’s immune system goes into overdrive in response to things normally present in the mouth, most often bacteria in plaque, but sometimes viruses as well. The result is widespread, painful inflammation that affects not just the gums but the inner cheeks, the back of the throat, and the tissue around the teeth.
This is not the same as regular dental disease, though the two can overlap. Think of typical periodontal disease as a localized problem around specific teeth. Stomatitis spreads through the entire oral cavity and doesn’t respond to standard dental cleanings alone.
Certain viruses, particularly feline calicivirus and herpesvirus, are frequently found in affected cats and are thought to contribute to the abnormal immune response. The exact cause isn’t fully understood, which is part of why treatment is so individualized. The surgery and diagnostics capabilities at Just Cats Clinic allow for a thorough workup right from the start.
How Do You Know If Your Cat Has Stomatitis?
Signs You Might Notice at Home
Cats are experts at hiding pain. By the time behavioral changes are obvious, the condition has often been building for a while. Here are the signs that should prompt a veterinary visit:
- Decreased appetite or refusing to eat altogether
- Weight loss
- Excessive drooling (called ptyalism)
- Pawing at the face or mouth
- Dropping food or chewing only on one side
- Crying out when yawning or opening the mouth wide
- Approaching the food bowl but then backing away
- A coat that looks increasingly unkempt from reduced grooming
- More hiding, irritability, or general withdrawal
Because these changes tend to develop gradually, they’re easy to dismiss. Regular preventive exams matter because a trained eye can spot early mucosal changes before things escalate.
What the Vet Team Looks For
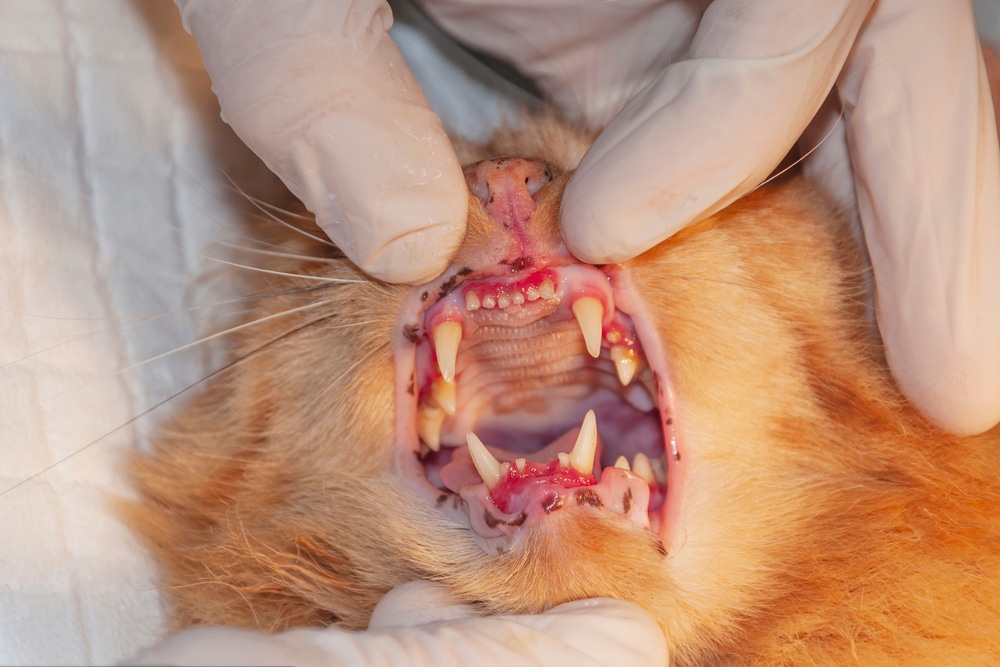
During a clinical exam, the veterinary team looks for specific changes in the soft tissues of the mouth. In cats with stomatitis, the mucosa is typically severely inflamed, ulcerated, and sometimes actively bleeding. The level of pain is usually significant, which is why a complete oral exam almost always requires sedation or general anesthesia.
Stomatitis vs. Dental Disease: Why the Difference Matters
Periodontal disease targets the structures that support the teeth: the bone, ligaments, and gum attachment. Stomatitis goes further, spreading to areas of the mouth that aren’t directly associated with the teeth at all.
Many cats have both conditions at once, which makes diagnosis more complex. Full-mouth dental radiographs are essential for getting the full picture. At Just Cats Clinic, complete radiographs are included with every dental procedure, helping the team assess root integrity, bone density, and any retained fragments that could be driving ongoing inflammation.
In cases where lesions look unusual or asymmetric, oral cavity tumors need to be ruled out. Oral tumors can look a lot like stomatitis but require a completely different treatment plan. If there’s any concern, a tissue biopsy is the right next step before moving forward with surgery.
What Does the Diagnostic Process Look Like?
Getting the diagnosis right sets the foundation for everything else. Here’s what a standard stomatitis workup typically includes:
- A full oral exam under sedation or anesthesia, with careful evaluation of all soft tissues and tooth structure
- Complete mouth radiographs to check for bone loss, retained roots, or anything abnormal
- Viral testing for feline calicivirus, feline herpesvirus, FeLV, and FIV, since these can affect both the disease course and the prognosis
- Bloodwork to assess organ function and overall health before anesthesia
Knowing whether your cat is a chronic calicivirus carrier, for example, directly influences what post-operative care will look like. Just Cats Clinic uses in-house lab capabilities alongside the IDEXX Reference Laboratory, so most results come back within 24 to 48 hours.
Treatment Options: From Medical Management to Surgery and Beyond
Can Medication Manage Stomatitis?
Medical management is often used in the early stages or alongside other therapies. Options typically include anti-inflammatory medications like corticosteroids, antibiotics such as amoxicillin-clavulanate or doxycycline, pain relief with NSAIDs or gabapentin, and sometimes antiviral medications like famciclovir or supplements like L-lysine to help address any underlying viral component.
Soft food can help cats with significant oral pain eat more comfortably. In severe cases, a temporary feeding tube ensures adequate nutrition while the team works toward a longer-term solution.
The honest limitation of medication is that it doesn’t fix the root problem. It can reduce inflammation temporarily, but the relief tends to become less effective as the disease progresses. Prolonged corticosteroid use also carries its own risks and can actually reduce the chances of a good surgical outcome down the road.
Full-Mouth Extraction: Still the Gold Standard
For most cats with confirmed stomatitis, full-mouth tooth extraction is the treatment most likely to produce lasting improvement. The logic is sound: by removing the plaque-retaining surfaces (the teeth themselves), the primary trigger for the immune reaction is eliminated.
Studies consistently show that 60 to 80 percent of cats experience substantial improvement or full resolution after complete extraction, with the best results in cats treated earlier in the disease process. It’s critical that all tooth root material is fully removed during the procedure. Retained root fragments can continue triggering inflammation even after an apparently complete extraction. Post-operative radiographs at Just Cats Clinic confirm that no root material remains.
All anesthesia and dental procedures include continuous monitoring of temperature, heart rate, blood pressure, and oxygen levels. Local nerve blocks are used to manage intraoperative pain, and a Class IV therapeutic laser is applied to soft tissue after extractions to reduce inflammation and support healing.
What About Cats Who Don’t Respond to Surgery?
Some cats continue to have significant inflammation even after full-mouth extraction, particularly those with active calicivirus involvement or a long history of medical management before surgery. For these cats, newer approaches are expanding the options.
Mesenchymal stem cell (MSC) therapy, specifically using adipose-derived stem cells (stem cells collected from fat tissue), is one of the most promising developments in refractory feline stomatitis. These cells are typically administered intravenously and work by modulating the immune response rather than simply suppressing it. Research into adipose-derived mesenchymal stem cell therapy has shown meaningful results even in cats who didn’t respond to traditional approaches, and outcomes may be further improved when MSC therapy is combined with existing medications.
MSC secretome is a related but cell-free option. It’s a concentrated, injectable preparation of the bioactive factors that stem cells naturally produce, including growth factors like EGF, VEGF, HGF, and others that help calm tissue inflammation. Because it doesn’t involve live cells, it’s easier to standardize and store.
Cryotherapy, which uses extreme cold to treat affected oral tissue, is another option being used in some cases. It can range from providing temporary pain relief to achieving more lasting resolution, depending on the individual patient.
Advanced antiviral and immunomodulatory combinations are also part of the evolving toolkit. For cats with confirmed viral involvement, medications like famciclovir paired with immune-modulating therapies can help manage the underlying trigger more effectively than antibiotics alone.
The team at Just Cats Clinic stays current with emerging treatment evidence and can help you understand which approaches might be most appropriate for your cat’s specific situation.
What Recovery Looks Like After Extraction
One of the most common worries owners have is how their cat will manage without teeth. The good news is that cats do remarkably well after full-mouth extraction. Most return to comfortable eating within a few weeks of recovery and often eat with more enthusiasm than they did before, because they’re no longer in constant pain.
Here’s what to expect in the post-operative period:
- Prescription pain medication for several days to weeks following surgery
- Antibiotics to reduce the risk of infection at extraction sites
- Soft food for the healing period, usually two to four weeks
- Monitoring of surgical sites at scheduled follow-up visits
- Medication adjustments as needed based on individual progress
Some cats, particularly those with calicivirus carrier status, will need continued immunomodulatory therapy after surgery. Your clinical team will discuss realistic timelines and revisit the management plan at each follow-up.
What Are the Long-Term Odds?
Early treatment consistently produces the best results. Cats treated surgically before extensive mucosal scarring or prolonged immunosuppression from steroids have the highest rates of complete resolution.
Factors that influence prognosis include:
- How long the disease has been present: Longer disease duration is associated with a less complete response
- Completeness of extraction: Retained root fragments are a leading reason inflammation persists after surgery
- Viral status: Active calicivirus infection may extend the recovery timeline and require ongoing management
- Individual immune response: A subset of cats will still need anti-inflammatory therapy long-term, even after successful extraction
Even in cats that require ongoing medication, the severity of pain and inflammation typically decreases substantially after surgery. Most owners see their cat return to eating, grooming, and engaging in normal daily life.
Keeping Cats Without Stomatitis Healthy
Stomatitis is a good reminder of just how central oral health is to a cat’s overall quality of life. For cats without the condition, consistent dental health habits go a long way toward preventing significant dental disease and catching early problems before they become serious.
At-home dental care can include regular brushing with CET Enzymatic Toothpaste and a CET Fingerbrush for cats who tolerate it. For cats who don’t love brushing, great alternatives include Vetradent Water Additive, Dental Care Powder, Greenies Dental Treats, ProDen DentalCare Bites, or Vetradent Dental Wipes for a lower-stress option.
Professional dental cleanings with full-mouth radiographs are recommended for most cats annually. The dentistry services at Just Cats Clinic are tailored specifically to feline patients, in an environment designed to minimize stress at every step.
Your Questions, Answered
Can stomatitis be managed with medication alone?
Medication can reduce symptoms in the short term, but it rarely produces lasting remission and typically becomes less effective as the disease progresses. Full-mouth extraction remains the treatment with the strongest evidence for sustained improvement, especially when performed early.
Will my cat be able to eat without teeth?
Yes, and often better than before. Soft food is required during the healing period, but most cats transition to eating normally within a few weeks. Many owners are surprised by how much more comfortable and engaged their cat becomes after surgery.
How long does recovery take?
Extraction sites typically heal over two to four weeks. The full inflammatory response may take several months to resolve completely. Follow-up visits allow the team to monitor healing and adjust the plan as needed.
What if my cat still has inflammation after extraction?
Some cats, particularly those with confirmed calicivirus carrier status, need continued therapy after surgery. Newer options like stem cell therapy and MSC secretome are showing real promise for these more complex cases. Your team will discuss what makes the most sense for your individual cat.
Is stomatitis contagious to other cats?
The condition itself isn’t directly transmissible, but the viral infections associated with it, such as calicivirus and herpesvirus, can spread between cats. Viral testing helps owners understand the risk and manage multi-cat households appropriately.
Getting Your Cat the Help They Need
Feline stomatitis is serious, but it is also a condition that can be managed, and for many cats, fully resolved. The cats who do best are those whose owners act early rather than waiting to see if things improve on their own. Oral pain affects everything, from how your cat eats and grooms to how they sleep and interact with you.
Just Cats Clinic is a feline-only, AAHA-accredited practice in Reston, VA with the expertise and resources to evaluate stomatitis thoroughly and guide you through every available treatment pathway. If your cat is showing signs of oral discomfort, please don’t wait. Schedule an appointment with our team, or contact the hospital to talk through your cat’s history and find the right next step.